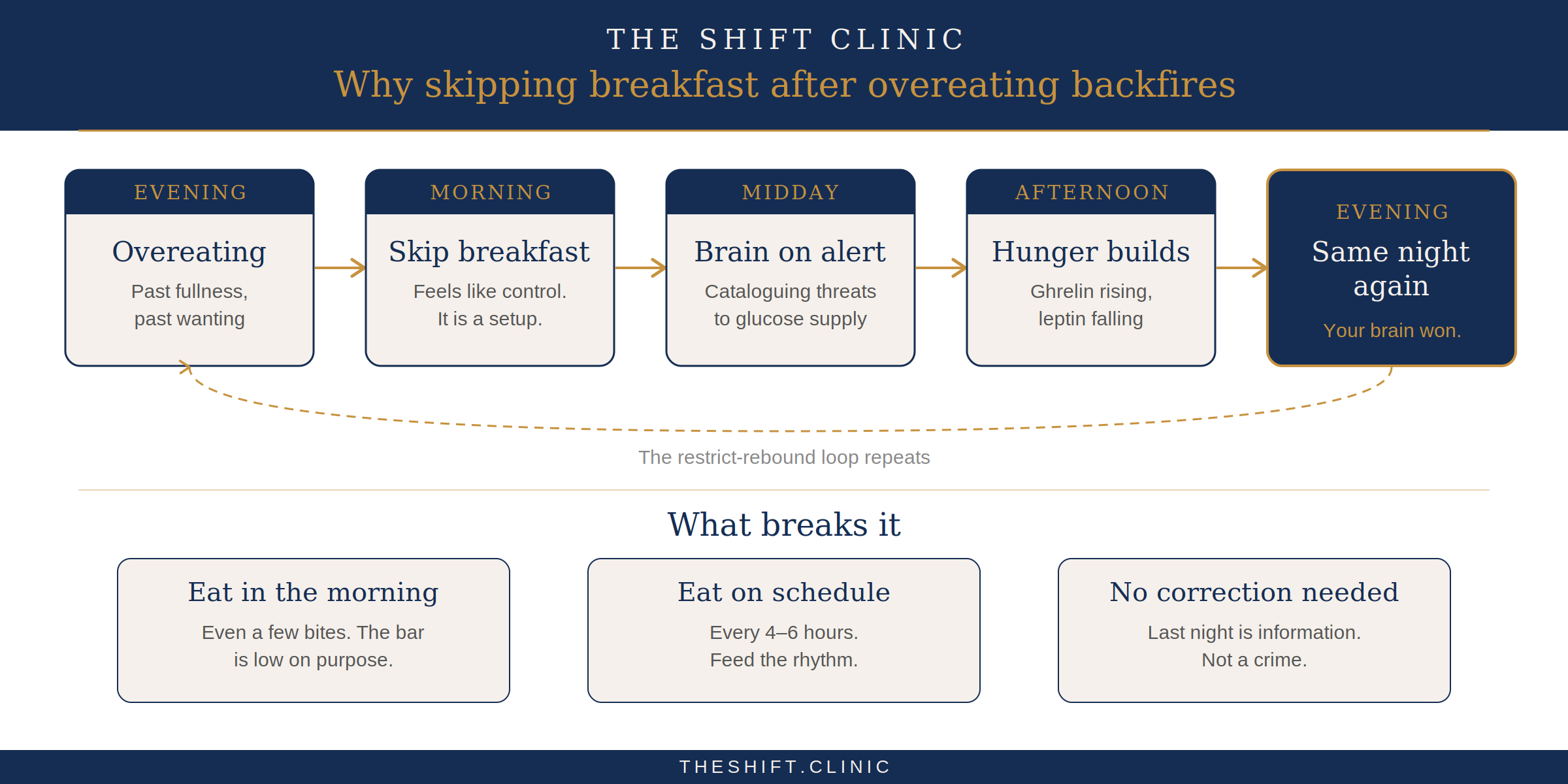
Your Brain Will Always Win That Fight: Why Skipping Breakfast After a Big Night Backfires
A patient sat across from me last week looking wrecked. Not sick. Ashamed. She'd eaten far past fullness, and well into wanting the night before. Not for a celebration or a social event. It was just another Thursday. She'd come home tired, opened the fridge, and by the time she surfaced it was 10pm and she felt terrible. Her plan for the morning was to skip breakfast. Start fresh. Earn back some ground by not eating.
I told her that was the worst possible response. Not because restriction is morally wrong. Because physiologically, it guarantees the exact same night again.
The correction instinct
You know the feeling. You wake up after a night of eating past full and your first thought is: I need to undo this. The logic feels clean. I ate too much last night, so I'll eat less today. I'll skip breakfast, maybe lunch, and by dinner I'll have balanced the books.
This is not a strategy. It is a setup.
When you don't eat all morning, your brain spends the entire day doing one thing: cataloguing threats to glucose supply. Your brain cares about two things on this planet, glucose and oxygen, and it has zero awareness of your long-term goals. It does not know you're trying to be disciplined. It does not care that you feel guilty. It is, and I say this with clinical respect, a dumb organ. And when you starve it to compensate for last night, it starts planning its counterattack by about noon.
By evening, you are right back where you were. Hungry past reason and eating everything you can see. Because your brain won. Your brain will always win that fight. The one to keep itself fed.
What's actually happening
Ghrelin, the hormone most associated with hunger signaling, rises before your habitual meal times and drops after you eat. It is entrained to your rhythm. When you skip that morning meal, you are not resetting. You are breaking the rhythm your body relies on to regulate appetite across the day.
Simultaneously, leptin, the hormone that communicates satiety to your brain, drops in response to energy restriction. Research has shown that even short-term fasting can suppress leptin significantly, which means your brain's ability to register "enough" gets worse precisely when you need it most. People with insulin resistance tend to have weaker accuracy around satiety signals specifically. They aren't worse at feeling hungry. They're worse at registering that they've had enough. So the system that was supposed to help you stop eating tonight just got dismantled by what you didn't eat this morning.
With fasting, your metabolism dips. Temporarily, but measurably. Your body interprets the absence of fuel as a threat and conserves energy in response. So you are hungrier, less able to perceive fullness, and burning fewer calories. That is not discipline. That is a trap.
The fasted-fed switch
Your body runs on a four- to six-hour cycle during waking hours. Fasted, fed, fasted, fed. That oscillation is how your organs know what to do. Your pancreas, your liver, your gut, your brain — they all depend on the signal of food arriving to switch gears. When you eat in the morning, even if you don't want to, even if the idea of food makes you feel sick, you flip the metabolic switch from fasted to fed as you eat.
This is not only about calories in versus calories out. Calories out is at least partially dependent on calories in. You can’t manipulate one side of the equation without having a counter-regulatory effect on the other. Feeding yourself is about restoring the fasted-fed rhythm so that the hormonal cascade that helps you move from hungry to full and round again can work. In this, your hunger signals show up at reasonable intervals, your satiety signals actually register, and your brain stops treating every moment as a glucose emergency.
Do not try to switch from Never Breakfast to Team Breakfast overnight. You will hate it. Start with just a few bites of food you enjoy. I don’t care what it is. The bar is low on purpose. The point is not to eat a large breakfast. The point is to tell your body that you will feed it, do so regularly, and go from there.
The medication layer
For people on weight loss medications, this matters even more. These medications work partly by suppressing appetite signals. Which is the point. But the side effect of suppressed signaling is that you can go hours without any feedback from your body at all, and then suddenly fall off a cliff. My patients describe it as feeling nothing for most of the day and then being hit by a wall of hunger that comes with shaking, headache, and a complete inability to make measured choices about food. It’s like not learning your house is burning until you see flames because you can’t smell smoke.
That is not the medication failing. That is the medication doing exactly what it was designed to do. And your job, especially on medication, is to eat on a schedule anyway. Not because you're hungry. Because your body needs the rhythm even when it can't tell you so.
The signals do come back. It takes time and practice. But they return faster when the body has a predictable fuel pattern to calibrate against.
Information, not a sentence
Back to last night. You ate past wanting. Maybe well past. Something was going on. A need for comfort that food temporarily met. In my practice, we call that eating into wanting. Your body had enough fuel, but your brain was still looking for something. That is information. It is not a crime. And where there is no crime, there is no need for punishment.
The instinct to restrict the next morning feels productive. It feels like you're taking control. But it deepens the confusion between fasted and fed states, amplifies the hunger cascade for the following evening, and reinforces the cycle that got you here.
Eat in the morning. Feed yourself. Let your body switch gears. Then eat again in four to six hours. And again. The rhythm builds itself back if you let it.
What my patient did
She ate breakfast. She didn't want to. She had a small protein shake, then made her coffee, which she very much wanted. By mid-morning, she noticed something unfamiliar: a mild, manageable hunger. Not panic. Not a drive-through emergency. Just a signal, arriving on time, saying it was time to eat again.
She ate lunch. And dinner was unremarkable. Not perfect. Just a normal evening where she ate until she was full and stopped. No correction needed.
That was the shift. Not a dramatic one. A small truce in the war she'd been fighting with herself for years. She did not need to earn her next meal.
If you're navigating appetite changes on medication, with insulin resistance, or after years of the restrict-overeat cycle, the Shift curriculum teaches the skills that make this livable. Not perfect. Livable.